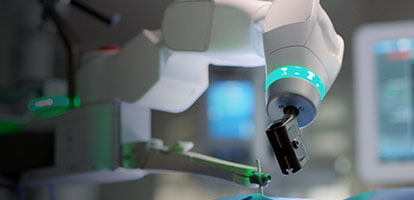
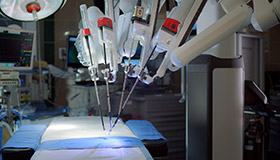
AHN is devoted to exploring, developing, and supporting innovations so that you have access to remarkable care, close to home. These robotic advancements, cutting-edge treatment plans, and breakthrough therapies are changing how we deliver care to give you the best possible outcomes.