AHN Neuroscience Institute experts treat neurological conditions, from headaches to brain tumors, with the most advanced treatments available.
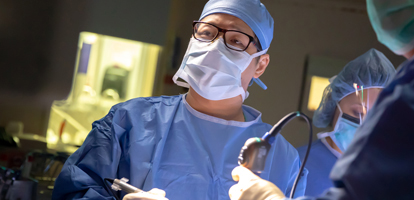
AHN Neuroscience Institute experts treat neurological conditions, from headaches to brain tumors, with the most advanced treatments available.
Conditions of the brain, spine, and nervous system can be confusing. We take the time to help you understand your options so you feel supported every step of the way.

One in three Americans is at risk for having a stroke. Learn 3 steps you can take now to protect yourself and help prevent a stroke.
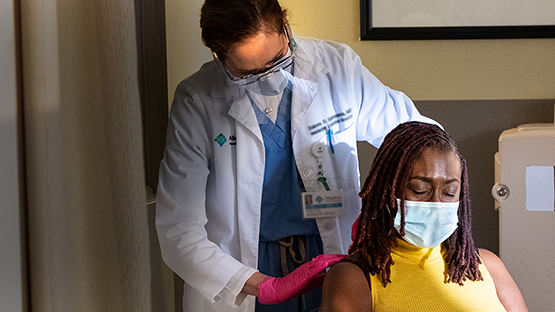
Our board-certified neurologists and neurosurgeons are leaders in their fields. Many physicians on our team have advanced training in the diagnosis and treatment of neurological conditions.
Our neurology and neurosurgery specialists have a high level of experience and skill in the evaluation and treatment of many different neurological conditions.
Using minimally invasive and robotic surgical approaches for serious spine and brain conditions can help some patients live a life with less pain.
With expert specialists and advanced capabilities, we provide comprehensive, effective treatments for even the most complex stroke conditions, fast.
Deep brain stimulation surgery has provided many patients substantial relief from tremors and other debilitating Parkinson’s symptoms.
Our headache specialists evaluate and treat people with migraines and other types of headaches to provide you with headache relief today and in the future.
We were the first health system in the United States to offer the new treatment Radicava®, an intravenous medication that may slow the progression of your ALS.
Our spine specialists use some of the latest surgical techniques and imaging technologies to help relieve chronic pain so you can get back to your life.

When his doctor controlled his erratic blood pressure, Carleton was no longer afraid of fainting and falling. Focused neurology care treated several troublesome conditions and changed his life.
Patients at the AHN Neuroscience Institute benefit from advanced treatment options, a team-based approach, and our commitment to research.

You have access to a team of board-certified experts who collaborate on diagnosing and treating complex conditions.

You’ll benefit from physicians dedicated to developing new treatments and participating in advanced clinical trials.
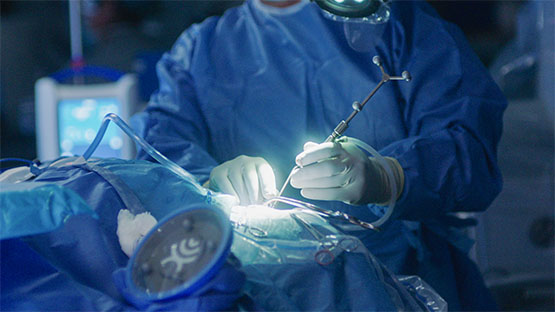
AHN’s renowned neurosurgeons have pioneered novel therapies that are changing lives, including:

Free for anyone, call anytime for around-the-clock support.
Call weekdays from 7:00 AM to 5:00 PM (closed weekends and holidays).
We are continually researching new ways to prevent, detect, and treat disease. Find specialists for your patient and discover educational opportunities for you.