Obstetrics and Gynecology Residency Curriculum and Didactics
Our curriculum combines robust clinical experience with comprehensive didactic teaching to develop trainees into compassionate, ethical specialty physicians and life-long learners who provide excellent patient care.
Clinical Training Overview
Clinical Rotations
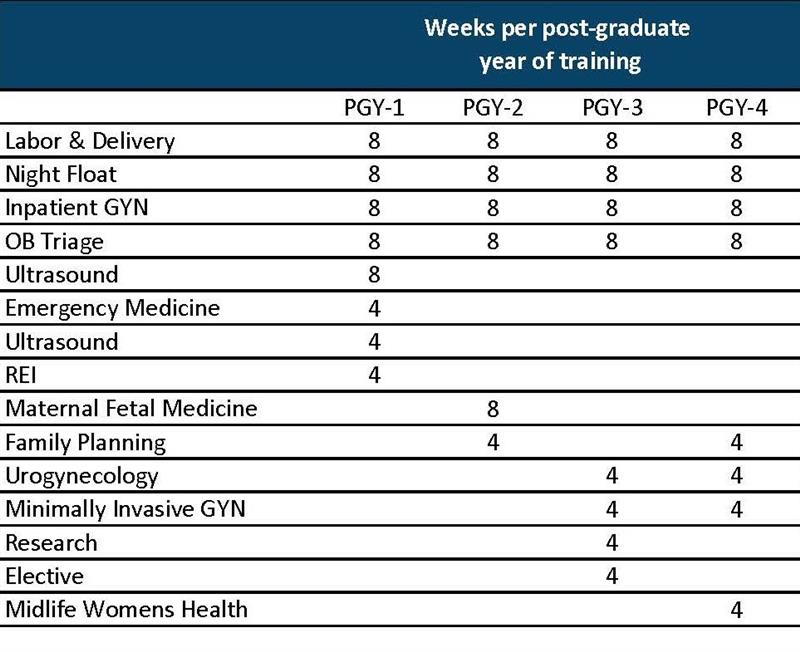
Resident rotations take place almost exclusively at West Penn Hospital, where residents benefit from the robust clinical volume in both normal and high-risk obstetrics, as well as gynecology and gynecologic subspecialties. Each of our inpatient services is also supported by mid-level providers, allowing residents to optimize their educational experience.
Beginning in PGY-1, residents attend a half-day continuity clinic session each week. The resident clinic has dedicated faculty and a consistent patient panel to maximize continuity for patients and providers. Additional outpatient exposure occurs integrated into each rotation, as well as during a dedicated Ambulatory Gynecology rotation.
Our educational objectives reflect those set by the Council on Resident Education in Obstetrics and Gynecology (CREOG), and our evaluation process includes 360 degree evaluations based on the ACGME Milestones. Residents take Step 3 and complete FLS certification during PGY-2. All PGY-4 residents are enrolled in a board review course as a part of preparation for written boards.

Didactic Education
Our didactic time is protected from clinical responsibilities, and includes one hour Tuesday Departmental Conferences as well as three hours of structured Resident Didactics on Fridays. Additional instruction occurs daily on clinical services. Our 24 month didactic cycle incorporates the CREOG educational objectives and includes a robust simulation curriculum. Our program values wellness, and a wellness curriculum and wellness time are included in our protected time.
Tuesday Morning Departmental Conference
- Grand Rounds
- Morbidity and Mortality Conference
- Practice Based Review of Literature
Resident Didactics
- Fetal Heart Rate Strip Review
- Outpatient Clinic Team Care Conference
- Structured Didactic Lectures and Case Based Learning
- Simulation Curriculum
- Wellness Curriculum
Monthly Journal Clubs, typically hosted by faculty

Ryan Foundation Grant
West Penn Hospital was awarded a Ryan Foundation Grant in 2017 and is committed to providing exceptional education in family planning care. We provide complex family planning services for many women in the region in our own institution as well as two freestanding clinics. We also tailor our curriculum for residents who "opt out," to create a rich learning experience and meet ACGME milestones.
Simulation Curriculum
Our simulation curriculum begins day one with Boot Camp, and spans all four years across obstetrical and gynecologic procedures and emergencies. Our curriculum is augmented by the state-of-the-art AHN STAR Simulation Center located next door to West Penn Hospital. Simulation training sessions occur during protected didactic time. Many simulation tools are also available to the residents outside of scheduled training sessions, including laparoscopic hysterectomy trainer with graduated skill modules, Da Vinci robot simulator, and Fundamentals of Laparoscopy trainer.




|
Obstetrics |
|---|
|
Intern Boot Camp Amniotomy Fetal Scalp Electrode OB Laceration Repair Spontaneous Vaginal Delivery Operative Vaginal Delivery Including Forceps Cesarean Section Breech Vaginal Delivery Postpartum Hemorrhage OB Emergencies and Codes 3rd and 4th Degree Laceration |
|
Gynecology |
|---|
|
Gynecologic Instrument Review Cystoscopy Hysteroscopy Operative Laparoscopy Myomectomy Total Laparoscopic Hysterectomy Robotic Surgery Manual Vacuum Aspiration Pelvic Floor Anatomy Intrauterine Device and NexplanonTM Placement |

Fundamentals of Laparoscopic Surgery (FLS)
The FLS training platform is located in the resident workroom to allow for convenient training between cases or while on call. Dedicated FLS training sessions are provided by MIGS faculty and other FLS certified faculty to ensure accuracy and efficiency in laparoscopic skills. Laparoscopic surgery skills are honed through graduated levels of responsibility with our specialty and subspecialty gynecologic surgeons.
Robotics Curriculum
All of our residents are capable of graduating with Certification of Da Vinci System Training. We begin formal didactics and robotics dry lab led by faculty beginning in PGY-1, and the Da Vinci training console is available for independent practice 24/7. Robotic surgery skills are honed through graduated levels of responsibility with benign gynecologic and oncology services.

