
Allegheny Health Network today announced that it is now offering a range of clinical, specialty services at a new location in Uniontown. The recently opened 27,500-square-foot multi-specialty outpatient center will enable care coordination at the site between Preferred Primary Care Physicians and AHN.
04/21/2024
04/20/2024
04/19/2024

Through Castle Connolly’s research process, about 67,000 board-certified physicians out of 985,000 practicing doctors across the United States have been awarded 2024 “Top Doctor” status, representing less than 7 percent of the nation’s physicians.

Russell Traister, MD, pediatric allergist at Allegheny Health Network’s Pediatric Institute, is providing helpful guidance for parents and caregivers this allergy season, as a mild winter now gives way to an early spring.
AHN is one of just 50 centers in the United States authorized to provide Amtagvi T-cell therapy
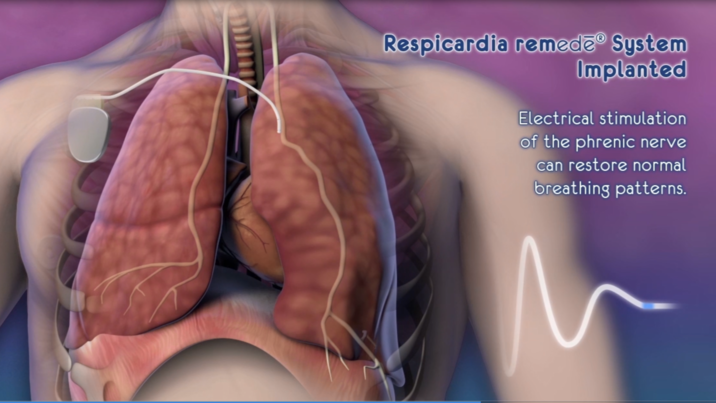
Allegheny Health Network announced today it is the first health system in western Pennsylvania to implant remedē, a pacemaker-like device that works to restore restful sleep for adult patients living with central sleep apnea.

Together, Joseph Ahearn, MD, Chau-Ching Liu, MD, Ph.D., and Susan Manzi, MD, MPH, of the AHN Autoimmunity Institute have been named ‘Inventor of the Year’ by the Pittsburgh Intellectual Property Law Association. The award is given annually to scientists whose patented developments have made significant, positive contributions to society.

Allegheny General Hospital was the top U.S. enrollment site for a landmark international clinical trial comparing the performance and durability of self-expanding and balloon-expandable transcatheter aortic valve replacements in patients diagnosed with aortic stenosis and small aortic annulus.

Allegheny Health Network and Highmark Health are investing more than $1 billion over the next several years in new construction and hospital expansions, to advance community access to affordable, high-quality health care in western Pennsylvania. View on YouTube how we are building the future of health care.

AHN podcasts share insights from health care pros and personal journeys from AHN patients. AHN apps can transform the way you receive health care, allowing you to review your medical information and connect with a doctor on your schedule.
Allegheny Health Network’s media relations team is dedicated to providing reporters and other members of the news media with the assistance they need.
By accessing this video, I understand that I am leaving the AHN website and I will be re-directed to an external website operated by a third party platform provider. I acknowledge that the platform provider may collect personal information about me, and about the video that I view, on their platform and may use and disclose this information in accordance with its privacy policy. I agree that Allegheny Health Network is not responsible for the data collection and use practices of this third party.