
Cancer Treatment Innovations
At AHN Cancer Institute, our team of expert researchers are driven by excellence. We use cutting-edge technology and groundbreaking therapy, tailored to each patient, for the best possible result.
Quick guide to AHN Cancer treatment innovations

CAR T-cell therapy for blood cancers
CAR T-cell therapy is offered at only a few cancer centers in the country. It’s an emerging treatment for aggressive blood cancers, including leukemia and lymphoma. CAR T-cell therapy involves taking blood from a patient and isolating the T-cells (disease-fighting immune cells). The patient’s T-cells are then reengineered into “fighter” cells using the CliniMACS Prodigy® machine on-site at AHN. This machine reduces fighter cell production time, and having this technology on-site also means the fighter cells never have to be frozen before being infused back into the patient. AHN is the first — and only — health system in the region to provide CAR T-cell therapy to patients with manufactured CAR T-cells under our own roof.
Learn more about our innovative blood cancer treatment and our personalized cancer treatment plans.
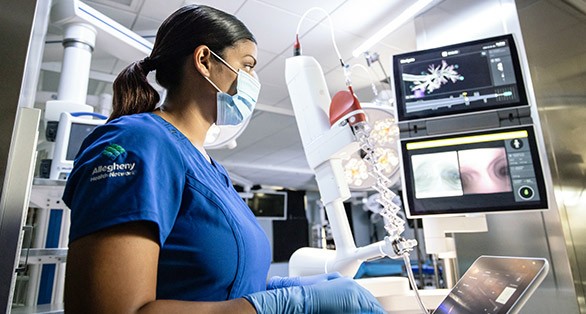
Ion™ Endoluminal System: Robotic lung biopsy helps detect lung cancer earlier
The earlier lung cancer is diagnosed, the better opportunity we have to successfully treat it. The new Ion™ Endoluminal System is a robotic scope that allows our doctors to grab tissue samples from deep within the lung, even around tight bends in the airways. AHN is the first in western Pennsylvania to perform lung biopsies with the Ion, which lets us detect and treat lung cancer earlier than ever before.
Our doctors use the Ion to access hard-to-reach tumors in a less invasive procedure than other biopsy options. We can then make a diagnosis by sampling tissue from small nodules in areas of the lung where previous tools and procedures couldn’t reach.
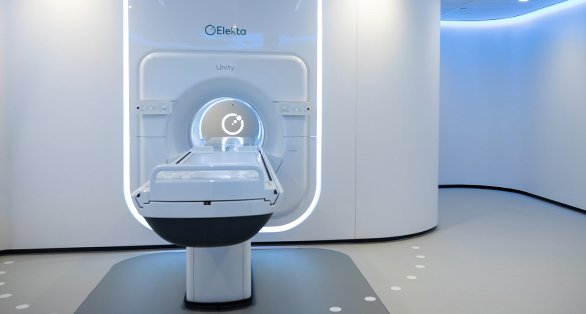
Elekta Unity MR-Linac: Precise and personalized treatment
MR-Linac is a breakthrough technology that simultaneously generates magnetic resonance images (MRI) and delivers radiation beams to the tumor tissue. Doctors view tumor tissue in real time and can adapt the radiation dose during the treatment.
The MR-Linac gives your doctor the ability to reshape the radiation dose based on daily changes in the shape, size, and position of the tumor and surrounding healthy tissue and organs — potentially resulting in better outcomes and fewer side effects.
The AHN Cancer Institute is one of the few facilities in the country to have the MR-Linac technology treatment option.
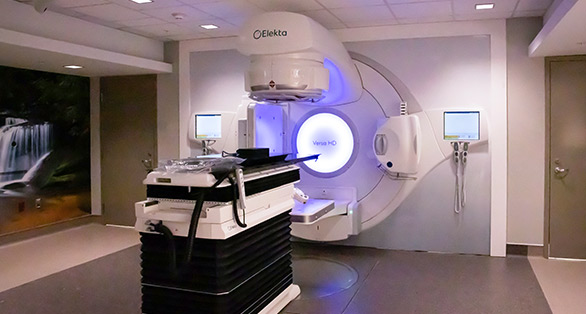
SBRT: Helping to manage liver cancer
Around 80% of patients with liver cancer aren’t eligible for surgery. However, stereotactic body radiation therapy (SBRT) is a nonsurgical procedure proven to shrink tumors in patients with inoperable liver cancer. It also serves as a bridge to liver transplants or eventual surgical removal. Slowing down tumor growth gives transplant-eligible patients more time to wait for a new liver to become available.
AHN Cancer Institute pioneered the use of SBRT as an option to safely treat these patients. Read how SBRT shrank Conny’s liver tumor.
HIPEC: Directed abdominal cancer treatment, application, and prevention
AHN Cancer Institute is one of the few centers in the country treating patients with advanced abdominal cancers using an innovative treatment called hyperthermic intraperitoneal chemotherapy (HIPEC). HIPEC's goal is to prevent new cancer growth with strong doses of heated chemotherapy, circulated directly in the abdomen. HIPEC can cause fewer side effects than intravenous chemotherapy. This approach is particularly effective for those with advanced abdominal cancers, as it is meant to kill microscopic cells left behind after surgery. Read about Gevony’s story with the HIPEC procedure.

Modus V: Enhanced precision in brain surgery
AHN uses the Modus V™* — a fully automated robotic digital microscope with a high-powered camera and light source that provides exceptional views of the brain. The Modus V’s features can potentially allow for the use of less-invasive brain cancer procedures, more rapid recovery, and reduced complications. This novel technology assists surgeons with extreme precision when removing brain tumors. Read how Dr. Williamson used the Modus V to remove Reba’s brain tumor.
Genomics Lab: Finding the genetic reason of tumor growth
Cancer is a disease of the genome. Our new DNA/Genomics lab with the AHN Genomics and Precision Medicine Center lets us explore each patient’s genes to see what’s driving tumor growth — and fight their cancer on a cellular level. When we’re armed with this information, patients get access to personalized cancer treatments at every AHN Cancer Institute location.
We use genome sequencing — or next-generation sequencing — to uncover the genetic changes unique to a patient’s particular tumor by analyzing the genetic sequence of tumor tissue and comparing it to the same individual’s normal (non-cancer) sequence.
Every person’s cancer is different, and every tumor has its own unique abnormalities at the genetic level. Some of these abnormalities, if identified, can be exploited to improve cancer detection, management, and treatment. The difference between the tumor and your normal sequences indicates where potential genetic abnormalities are and they may make cancers vulnerable to a particular drug or therapy.
OsteoCool: Managing spinal tumors with heat
OsteoCool™* is a minimally invasive option for patients who need complex spinal reconstruction surgery. OsteoCool uses radiofrequency energy to kill painful spinal tumors. Surgeons make two small puncture incisions and then transmit heat energy into the tumor. This minimally invasive technique has resulted in patients receiving immediate pain relief. Read Leo’s story about how OsteoCool made his back feel as good as ever.
Immunotherapy: Boosting the immune system's ability to beat cancer
Immunotherapy improves the immune system’s ability to target cancer cells and stop or slow their growth. AHN Cancer Institute oncologists offer immunotherapy to effectively treat many types of cancer, often in combination with other forms of treatment. Read how Claud turned to immunotherapy for his stage 4 lung cancer.

VECTRA® WB360
This breakthrough machine takes 92 photos of your skin from head to toe to create a computerized 3D model. It gives doctors a close-up view of every mark and every mole to track changes year to year, spot skin cancer early, and treat it effectively. It’s the most accurate mole-tracking system available. There are only a handful of these machines in the country, and one of them is at AHN.
Contact us
Call the Hope Line at (412) 578-HOPE (412) 578-4673 to connect with a nurse navigator or schedule an appointment.
-
Appointments
Cancer Institute(412) 578-HOPE
VECTRA® is a registered trademark of Canfield Scientific, Inc.
By accessing this video, I understand that I am leaving the AHN website and I will be re-directed to an external website operated by a third party platform provider. I acknowledge that the platform provider may collect personal information about me, and about the video that I view, on their platform and may use and disclose this information in accordance with its privacy policy. I agree that Allegheny Health Network is not responsible for the data collection and use practices of this third party.

