
Newsroom
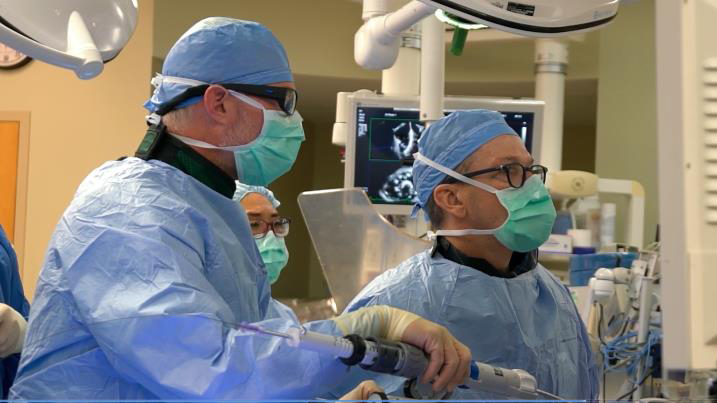
Cardiac Surgeons at Allegheny General Hospital First in Region to Successfully Perform Transcatheter Tricuspid Valve Replacement Procedure
Friday, February 20, 2026
Cardiac experts from Pittsburgh’s Allegheny Health Network’s (AHN) Allegheny General Hospital (AGH) announced today they are the first in the region and among the first in the state to successfully perform a transcatheter tricuspid valve replacement (TTVR), a minimally invasive procedure used to treat a complex heart condition known as tricuspid valve regurgitation.
AHN in the News
-
Educators explain CHILL Room
Mar 13, 2026
-
Pittsburgh woman shares message after Lyme disease diagnosis
Mar 13, 2026
-
Will ultrasound be future of fighting cancer?
Mar 12, 2026
-
Erie hospital offers new surgery for chronic lower back pain
Mar 11, 2026
-

Beyond Diagnosis: How Allegheny Health Network’s Innovative Personalized Care is Redefining Life with MS
Tuesday, March 17, 2026
In recognition of Multiple Sclerosis Awareness Month, discover how AHN's personalized approach empowers patients to live well with this chronic neurological disease, impacting over 1 million people in the United States.
-
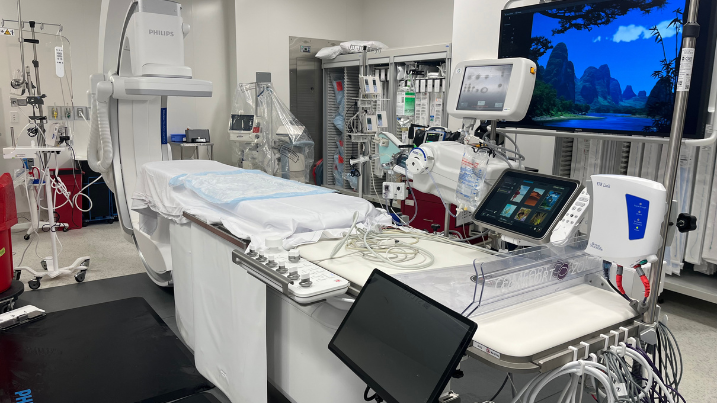
Allegheny Health Network Opens Second, State-of-the-Art Cardiac Catheterization Lab at Forbes Hospital
Thursday, March 12, 2026
New cath lab expands access to advanced, life-saving heart care for patients in eastern Allegheny County
-

AHN Cancer Institute - Forbes to Host Saturday Cancer Screening Clinic on April 18
Wednesday, March 11, 2026
AHN Cancer Institute will host its monthly Saturday cancer screening clinic on Saturday, April 18, at AHN Cancer Institute – Forbes
-

Allegheny Health Network’s Cardiovascular Institute Opens Clinic Dedicated to Congenital Heart Disease in Adult Patient Populations
Friday, March 06, 2026
AHN Allegheny General Hospital today announced the launch of its comprehensive Adult Congenital Heart Center, a regional resource for patients with abnormal heart chamber structures, holes in the heart, malformed valves and other heart defects.
-

AHN Prehospital Care Services announces AHN Canonsburg Ambulance Service Designated as Primary Provider for Peters Township
Wednesday, March 04, 2026
Allegheny Health Network (AHN) Prehospital Care announced today that AHN Canonsburg Ambulance will soon be serving as the primary emergency medical services (EMS) provider for Peters Township.
-

Dr. Ashley M. Carlucci Named Chief Nurse Executive for Allegheny Health Network
Wednesday, March 04, 2026
Allegheny Health Network (AHN) today announced the appointment of Ashley M. Carlucci, DNP, MHA, RN, CEN, CENP, as its new Chief Nurse Executive (CNE), effective April 13.

Building the future
Allegheny Health Network and Highmark Health are investing more than $1 billion over the next decade in new construction and hospital expansions, to advance community access to affordable, high-quality health care in western Pennsylvania.

AHN Apps and Podcasts
AHN podcasts share insights from health care pros and personal journeys from AHN patients. AHN apps can transform the way you receive health care, allowing you to review your medical information and connect with a doctor on your schedule.
Are you a media professional?
Allegheny Health Network’s media relations team is dedicated to providing reporters and other members of the news media with the assistance they need.
By accessing this video, I understand that I am leaving the AHN website and I will be re-directed to an external website operated by a third party platform provider. I acknowledge that the platform provider may collect personal information about me, and about the video that I view, on their platform and may use and disclose this information in accordance with its privacy policy. I agree that Allegheny Health Network is not responsible for the data collection and use practices of this third party.

